Innovative Approaches to Maternal Care in Rural Alabama: The Role of Robotic Ultrasounds
Addressing Rural Healthcare Challenges with Technology
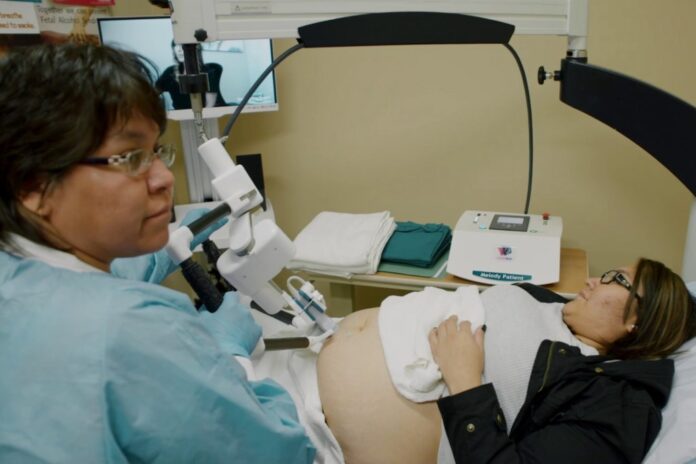
What once seemed like a concept from futuristic fiction is now being explored in Alabama, where state officials are considering the use of robotic technology to enhance prenatal care for pregnant women in remote areas. This initiative aims to tackle the persistent shortage of healthcare providers in rural communities by integrating advanced tools such as robotic ultrasounds.
Mixed Reactions to Robotic Ultrasound Implementation
During a January White House roundtable highlighting the initial grants from a $50 billion federal rural health fund, Mehmet Oz, Administrator of the Centers for Medicare & Medicaid Services, praised Alabama’s robotic ultrasound proposal as an exciting innovation. However, the idea sparked controversy, with Senator Bernie Sanders criticizing it as inadequate and some healthcare professionals expressing concerns about the implications of replacing human care with machines. This debate underscores the tension between embracing cutting-edge technology and addressing the fundamental lack of healthcare personnel in underserved regions.
Current State of Maternal Healthcare in Alabama
Alabama faces significant challenges in maternal and infant health. In 2024, the state’s infant mortality rate stood at 7.1 deaths per 1,000 live births, notably higher than the national average of 5.5, according to provisional CDC data. The decline in hospital-based obstetric services has been dramatic: from 45 rural counties offering such care in 1980 to only 15 projected by 2025. This reduction has been exacerbated by the closure of five obstetric units in 2023 and 2024 alone, including in Monroe, Marengo, and Clarke counties.
Expert Perspectives on Robotic Ultrasounds and Workforce Needs
Britta Cedergren, director of the Alabama Perinatal Quality Collaborative, emphasizes that while robotic ultrasounds represent promising technology, they are not yet in active use within the state. Instead, healthcare providers rely on telehealth and phone consultations where possible. Cedergren stresses that technology cannot replace the necessity of a skilled healthcare workforce and a well-coordinated system for maternal and fetal care.
Similarly, Dr. LoRissia Autery, an obstetrician-gynecologist serving rural Alabama, voices concerns that robotic ultrasounds cannot substitute the nuanced care required for high-risk pregnancies, which often involve complications such as diabetes and hypertension. Her clinic, Walker Women’s Specialists, serves patients across five counties and struggles to recruit additional physicians, highlighting the broader workforce shortage.
National Context and Alabama’s Unique Approach
Nearly every state applying for the Rural Health Transformation Program identified workforce shortages and maternal health as critical issues. However, Alabama stands out as the only state proposing robotic technology as a solution to bridge these gaps. The state received $203 million for the program’s first year, with plans to invest in both workforce development and technological innovations to improve rural maternal care.
International Examples: Successes in Remote Healthcare Delivery
Canada offers a compelling model for integrating robotic ultrasounds with human expertise. In La Loche, Saskatchewan, nurse practitioners operate robotic ultrasound devices connected to remote sonographers and radiologists. This system reduces the need for patients to travel long distances-up to six or seven hours-to access specialized care. Research from the University of Saskatchewan found that 70% of telerobotic ultrasounds eliminated the necessity for travel, with high patient satisfaction reported.
Dr. Ivar Mendez, director of Canada’s Virtual Health Hub, notes that while robotic ultrasounds are effective for many prenatal assessments, they cannot replace all types of ultrasounds, such as invasive vaginal scans. The northern regions of Canada still face maternal and infant mortality rates 20 to 25 times higher than the national average, largely due to limited access to prenatal imaging.
Technology and Training: Alabama’s Dual Strategy
Alabama’s Rural Health Transformation Program includes a comprehensive plan to connect smaller rural providers with regional centers capable of delivering high-quality maternal and fetal health services digitally, including through telerobotic ultrasounds. Alongside this, the state aims to enhance workforce capacity by investing in training programs for doctors, emergency responders, and nurse-midwives.
The maternal and fetal health initiative is projected to require $24 million over five years, while workforce development efforts are budgeted at approximately $310 million for the same period. These investments reflect a recognition that technology must complement, not replace, a robust healthcare workforce.
Looking Ahead: Balancing Innovation with Human Care
While robotic ultrasounds offer a promising tool to extend prenatal care into underserved rural areas, experts caution that they cannot fully substitute the personalized attention provided by trained healthcare professionals. Alabama’s experience highlights the complexities of integrating advanced technology into healthcare systems facing workforce shortages and infrastructure challenges.
As the state moves forward with its rural health initiatives, ongoing evaluation and adaptation will be essential to ensure that innovations like robotic ultrasounds enhance, rather than diminish, the quality of care for mothers and infants in rural communities.